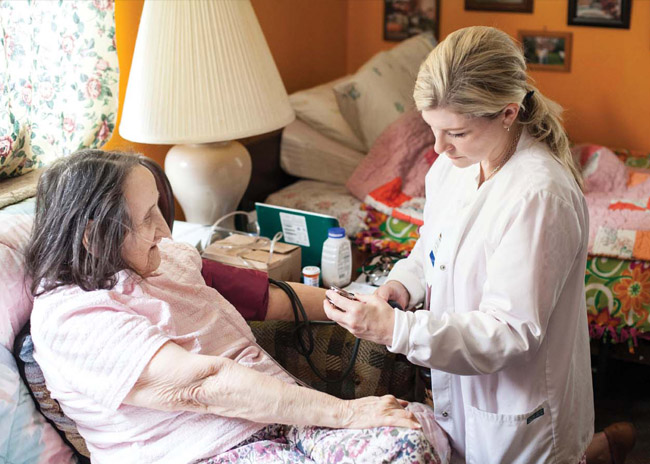
For people with a chronic illness, leaving the hospital after an acute episode can be overwhelming, confusing and scary.
They have many medications to juggle, may struggle to remember their providers’ instructions, and have to fight social barriers like transportation to the pharmacy or grocery and missed work or school days.
With all of these issues, many return to the hospital after only a few days. If only there were some way to help these patients better connect the dots of their care.
Vanderbilt University School of Nursing is piloting two projects—one in pediatric asthma and one in heart failure—that aim to improve transitions of care and keep patients out of the hospital.
“Let’s build a bridge, but let’s make it one way—out of the hospital and into the home and primary care clinic. We don’t want patients in that ravine where no one is keeping track of them,” said Natasha McClure, MSN, instructor in the Community Health Nursing and PreSpecialty Program, who leads the asthma project.
The asthma and heart failure care transition projects are part of the clinical component of the community health course for students in the PreSpecialty component of the MSN program, the generalist nursing series of classes students take before progressing to their specialty level of education. Pairs of students are assigned a patient and make home visits to assess their needs, identify barriers and facilitators and create health goals.
“These services are an extra resource. We emphasize that our clinical interventions do not replace a home health or clinic visit. We are simply an extra set of eyes and ears and can give some insight into what is happening in the home that may be causing some of these hospital readmissions,” said Melissa Smith, DNP, ANP-BC, adult-gerontology primary care nurse practitioner program instructor, who leads the heart failure project.
About 5.8 million people in the U.S. have heart failure, and half of people who develop it die within five years of diagnosis. According to the American Heart Association, about 1 million people are hospitalized with heart failure each year, and one-fourth of those return within 30 days.
The average heart failure patient is on six medications to treat just one disease. It is a progressive disease that requires management of many factors, including diet, fluid balance and medications.
That’s where the nursing students’ extra eyes and ears can be so valuable.
“The students are able to go into the medical record and see which medications the patients have been prescribed at the time of discharge. They go into the home and work with the patient to determine what they are actually taking. They help patients understand the importance of weighing every day to monitor their fluid balance and make sure they are looking for signs and symptoms,” Smith said.
In turn, the students are getting an insight into the factors affecting the transition of the patient from hospital to home.
“We’re raising the bar for these students immensely, and they’re going above and beyond normal work for the community health course,” Smith said.
Students utilize a specific home visit guide related to CHF or asthma and learn how to individualize a patient’s health history and write a SOAP (subjective, objective, assessment and plan) note. A Promise of Nursing grant, from the National Student Nurse Foundation, provided cell phones for students to be able to contact patients and iPads for face-time with the faculty in the home and to display a voice-over PowerPoint presentation during the home visit. Another grant from Vanderbilt’s Medical Center Staff Advisory Council purchased low-literacy education materials and weight scales.
“We grew and learned a lot in the initial phase. It was a lot of hands on, and I felt like we all became very independent by the end,” said psychiatric-mental health specialty student Anna Reiff.
But Reiff recognized that it took a lot of investment and patience to see any results.
“We didn’t see the fruit of our labor right away. (Our patients) have to get to know us and we have to get to know them. Eventually, we could tell when they went up in weight and could know what they needed because we were consistently interacting.”
After following her patient every two weeks for a year, Reiff said it was hard to say goodbye.
“My patient said we made such a difference and she wouldn’t be where she was without us.”
Marian Dudley knows that feeling. She has had heart failure for about 10 years and has known Professor Smith from her work in Vanderbilt’s heart failure clinic. Dudley, 76, was thrilled to participate in the pilot program and welcomed students into her East Nashville home.
“We go way back,” Dudley joked to Smith, when she checked up on her in late July while the nursing students were on summer break.
“She has been a big lifesaver to me. She got my meds straightened out and got oxygen for me.”
Dudley says her legs feel like rubber and she gets short of breath easily, but otherwise feels pretty good. Smith assesses her needs and determines the assistance she needs such as home health visits and who is picking up her groceries and doing the housekeeping. She also checks Dudley’s blood pressure, listens to her heart and lungs and looks over her weight log.
If there were any red flags, Smith would contact Dudley’s cardiologist. Today, with everything looking good, they can talk about homegrown vegetables and how much Dudley loves to watch the television show “Ellen.”
“Most of the time it’s helpful just to talk to someone,” Dudley said.
With the first year of project implementation completed, Smith is refining the program to identify the patients who could benefit most, developing the discharge criteria, and deciding which factors should be measured to determine the success of the intervention.
“We had one patient with six admissions, four of them fewer than 30 days apart. After we were involved, he had one admission, and it was greater than 30 days. He did not have a readmission from April until August,” Smith said. “On the other hand, there are some patients we haven’t been able to impact no matter what we do. We are learning about the factors that impact early readmission.”
According to the Tennessee Department of Health, 10 percent of children in Tennessee have asthma, and it is the most common chronic disease of childhood worldwide. An emergency department (ED) visit for an asthma attack creates chaos for the family, and can be dangerous for a child as they are exposed to other illnesses, like cold and flu. Uncontrolled asthma may lead to missed school days, poor quality of life and risk of sudden death.

“I worked in the ED and have seen these children in respiratory distress. It’s often preventable, and it’s upsetting when the parents don’t know how or don’t have the resources to get the child’s asthma under control, and that child is suffering as a result,” McClure said.
Many acute asthma attacks are preventable through consistent medication use and environmental factors, but busy parents often don’t have the time or resources to manage it well. McClure encourages nursing students to treat their home visit like an investigative mission.
“Two of the big triggers for asthma are cockroaches and mold. Many of our families are in Metro Nashville (subsidized) housing and it’s a hard problem for them to overcome by themselves,” she said. “For a single mom with several children, just getting to school on time is hard. So we help make a schedule and put a chart on the refrigerator to help them remember medications and keep track of their usage.”
McClure received a grant from the Medical Center Staff Advisory Council to purchase HVAC filters, cockroach treatment, pillow and mattress covers and inhaler dose counters.
“With $1,000 we funded eight families last year, and each visit to the ED costs around $5,000. We’ve found that a small investment can help a few families and save not just money, but children’s lives,” she said.
The biggest lesson learned is that there is no magic solution for every patient.
“Every patient is different, and we provide individualized care. Something floats to the top for every patient, but it’s not the same for everyone.”
That’s why home visits are so important. The students and families can get comfortable with one another and be more open and honest.
“We don’t go in and tell them everything they’re doing wrong. We want to reinforce the positive things they are doing, and really try to make them feel like we are part of a team, along with the entire family,” McClure said.
Family Nurse Practitioner/Midwifery student Rosalind Elliott said it was rewarding to establish a relationship and create a safe space for the families to open up.
“Once they were comfortable, they would say it was hard to give the medication in the morning because they have other kids and are just trying to get to school on time. But we never heard that on the first visit. It was important to be on their turf and let them know we understand the challenges and see how hard this is every day,” Elliott said.
“It was different seeing it from that side,” added Women’s Health student Chelsie Hochradel. “We sit in the classroom and talk about needy communities, but these patients let us in their home to see what isn’t connecting. It was really rewarding.”
Home visits also allow more time for teaching.
“Our students get a two-hour lesson on asthma and would probably still say it is confusing. Families get 30 minutes in the clinic to learn how to take their medicines correctly and what to do if they have an exacerbation,” McClure said. “We’ve found that repetition is key—just going over all those instructions again and again.”
The students also provided helpful exercises to show how difficult breathing with asthma could be. They had parents and siblings puff through a straw and then pinched the straw to simulate an asthma attack and added a little ball of Play-Doh to mimic the blockage that builds up gradually as a result of inflammation.
Seventeen families have participated in the program over two years, and results have been very positive. McClure says one patient had eight emergency department visits in four months, and had none for the two years they were followed by the student group.
“Since our health care system needs to shift from acute care to primary care and preventative care, we need to teach nurses how to better take care of patients with chronic disease,” McClure said. “Our model is asthma, but it could be applicable to diabetes or heart failure or obesity. It looks slightly different in each, but it’s the same core system and skills.”
And the students will carry those skills into their future practice.
“I want to make sure people know I’m listening and want to be there to help,” Hochradel said.
“I saw that chronic illness is a constant crisis mode of living,” Elliott added. “I learned that trust takes time, and the space you practice in matters. It’s important to be aware of the intimidation factor. This was a positive power shift because we could meet in the middle in someone’s home.”
Melanie Lutenbacher, PhD, MSN, FAAN, associate professor of Nursing and Medicine, who helped with the refinement and evaluation of these projects, said overall they are a win-win-win—for patients, hospitals and students.
“By creatively leveraging resources from VUSN, the Medical Center and the community, these teams have created an innovative system of care for complex patients—improving their quality of life and reducing risk of readmissions, and providing our nursing students excellent ‘real world’ learning opportunities,” Lutenbacher said.
Often all that is needed to bridge the ravine is a trained eye and a listening ear.