Without a way to effectively monitor and measure swelling in limbs, breast cancer patients with lymphedema can have difficulty with self-care and knowing when to seek treatment.
Vanderbilt University School of Nursing’s Sheila Ridner, PhD, RN, and her team hope to change that with a new study that could lead to objective measuring at home and improved self-care.
There are approximately 2.3 million breast cancer survivors in the United States and lymphedema, or swelling in the arm, occurs in up to 40 percent of those patients.
“People with diabetes have glucometers at home to measure their blood sugar, but right now, the only way patients with lymphedema can measure their arms is through water displacement – actually dunking their arm in water and measuring the water outflow or by holding a tape measure and trying to ascertain girth,” said Ridner. “These patients need a better way.”
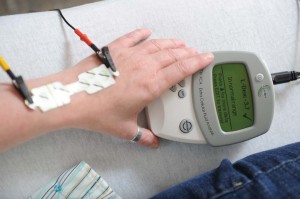
Enter the two-phase grant Ridner secured from the National Institute of Nursing Research to develop a protocol for home monitoring using a bioelectrical impedance tool, a hand-held device that connects to a patient’s arms using electrodes and provides a measurement for extra cellular fluid. The device will provide a lymphedema index ratio (L-DEX) ranging from 1 to 40.
The first phase is a developmental study to test and refine draft protocols for patient use and determine measuring schedules. During this phase, daily arm measurements will be collected for 10 days from women with and without lymphedema to compare swelling measurements.
“We really don’t know if the extracellular fluid varies more or less in an arm with lymphedema or without lymphedema. This will be the first time the measuring equipment is used over time in both populations to study this,” said Ridner.
The second phase is a small clinical trial of breast cancer survivors with lymphedema. Half will be randomized to use the measuring device for three months at home using the new protocol and sending back volume readings.
The other half will not use the measuring device. Both groups will document whatever they are doing for self-care and any lymphedema symptoms for three months. Any participants with increased arm swelling will be referred to the Vanderbilt-Ingram Cancer Center’s new Vanderbilt Lymphedema Therapy Clinic.
“We want to see if people who actually measure do more or less self-care, and we are going to follow economic issues such as arm infections and expenses for lymphedema treatment. Part of the patient frustration with self-care is that they can’t tell if it works or if self-care reduces arm problems,” said Ridner.